When will the blood clot become dangerous
When we were injured and started to bleed ourselves, our body was able to stop bleeding quickly by creating clots that clogged the wounds. This reaction is very important because it ensures that we minimize the loss of blood, prevent bacteria from entering the wound and healing the wound.
However, even in the absence of trauma, blood clots are sometimes formed in the bloodstream and the blood vessels may be blocked. This type of blood clot rarely occurs, but some diseases and genetic factors increase the risk of thrombosis. Many people with this high risk use anticoagulant drugs as a preventative measure.
When we hurt ourselves and start to bleed, this is what happens.
This reduces blood flow to the injured tissue, limiting the loss of blood.
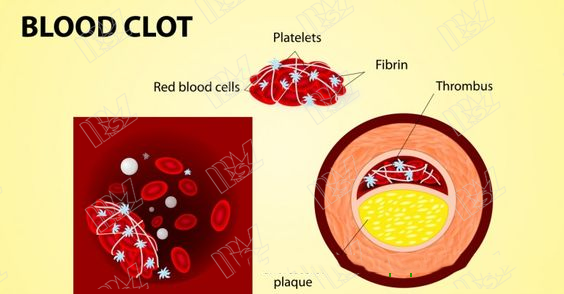
Platelets in the blood, attach to damaged areas of blood vessels and come together to reduce bleeding.
The body then activates some of the blood and tissues. These substances cure the clumps by forming special proteins and fixing the lump at the wound. These substances are called clotting factors. Most of them are made in the liver. The liver needs vitamin K to make some clotting factors. Our bodies can not make their own vitamin K, so people have to put their diet on.
For example, blood flows too slowly and starts to accumulate, and large numbers of platelets may aggregate to form blood clots. If the clotting factor is stronger, it also increases the risk of clot formation, which is not sure. This can happen for many reasons, including genetic predisposition, cancer, or because someone is taking some type of medication. The medical term for clots is "thrombus."
When will the blood clot become dangerous?
If a blood clot is formed in the vein, it is called venous thrombosis. One of the main causes of this thrombus formation in the legs is that there is not enough exercise for a long period of time - probably because they have undergone major surgery or have had a serious illness or injury. If some of the blood clots, called emboli, fall off and block the blood vessels in the lungs, blood clots in the legs can become dangerous. For this situation is the pulmonary embolism. Typical symptoms of pulmonary embolism include severe breathing problems, cough, hemoptysis, and chest pain.
If arterial thrombosis occurs, the tissues and organs they usually supply no longer have enough blood, or no blood at all. This thrombus usually occurs in the coronary arteries or inside the heart. If the thrombus blocks the coronary arteries, it can cause a heart attack. A blood clot in the heart itself can cause a stroke if it moves to the brain and blocks blood vessels.
Patients with atrial fibrillation have a higher risk of thrombosis in the heart. Atrial fibrillation is a special type of arrhythmia, in which two rooms (called the atria) beat very rapidly and irregularly. This means that blood does not flow through the prosthetic heart valve also increases the risk of thrombus: their surfaces are not as smooth as the native valve, so platelets are more likely to attach to them and form blood clots.
Specific medications or diseases such as cancer or hereditary coagulopathy also increase the risk of clot formation.




 Price is 8-20% Lower Than Other
Price is 8-20% Lower Than Other






