Mini ultrasound and stethscope-which is better?
Mini ultrasound is already a valuable adjunct to the stethoscope and plays an important and increasing role in medical education and physical diagnosis. So which is better, mini ultrasound or stethoscope?
" mini ultrasound technology is far superior to the stethoscope in the ability it provides to an experienced user in rapidly 'ruling out or ruling in' certain key diagnoses, immediately, at the patient's bedside," Dr. Sharon L. Mulvagh, MD, FRCP(C), and Dr. Anjali Bhagra, MBBS say.
"People like to compare ultrasound to the stethoscope, but ultrasound is actually a much more powerful tool when used well," Christopher L. Moore, MD, RDMS, RDCS, associate professor of emergency medicine at Yale University School of Medicine in New Haven, Connecticut, told Medscape Medical News. "Like the stethoscope, the contribution to diagnosis is directly related to the skill of the operator."
From the perspective of cost and feasibility, previous impediments to widespread use of ultrasound have included their cost and size. The development of faster microprocessors and better miniaturization has recently allowed fully functional ultrasound machines in laptop computers, or even as handheld devices that fit in a coat pocket. As the price of mini ultrasound devices has fallen, they are now more accessible to physicians other than radiologists and cardiologists.
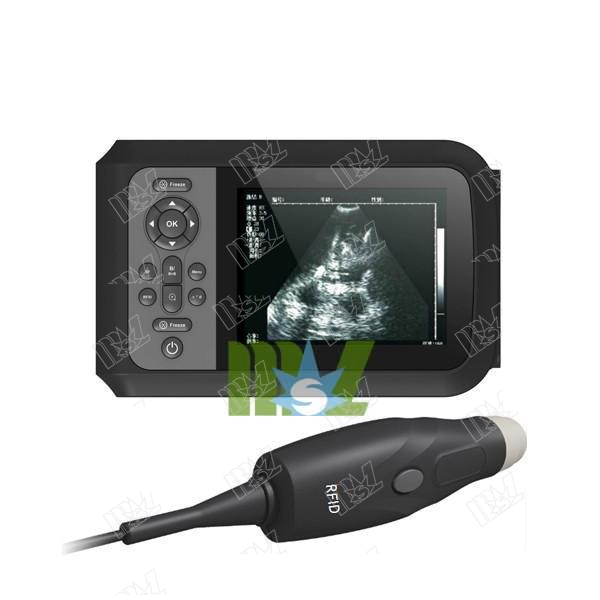
"We are advocating that mini ultrasound devices be used as an extension of the stethoscope, and not a replacement for the stethoscope," Dr. Mulvagh and Dr. Bhagra said. " mini ultrasound is intended to enhance the physical examination by actually 'seeing,' or 'not seeing' (ruling in or out) the suspected pathophysiology from a carefully performed clinical assessment."
However, it is not easy to widespread mini ultrasound use. Problems include possible reservations by specialists already trained in ultrasound use and interpretation, issues regarding medical records and billing, false-negative as well as false-positive results, and potential distraction of medical students from the core principles of physical diagnosis.
"It is important that when ultrasound is used as a focused diagnostic test in an appropriate situation that it be reimbursed appropriately, even when done by nonradiologists," Dr. Moore said. "This will help to ensure quality and provide the resources for equipment and teaching that are needed to do it well."He noted that false-negatives and false-positives caused by less-experienced operators will decrease with more practice and exposure and should not unnecessarily limit mini ultrasound use.
"At the same time, it is important that people using ultrasound receive good training and understand their limitations, that strong policies are in place about what can and should be done with ultrasound [and] by whom, particularly when ruling in or ruling out a diagnosis, and that patients also are made aware of the difference between a point-of-care ultrasound and a comprehensive study," Dr. Moore added. Dr. Narula and Dr. Nelson also recommend supervision for any diagnostic decisions made by trainees, whether for ultrasound or for physical examination.
"Overconfidence in ultrasound results could lead to unnecessary additional testing or premature diagnostic closure when test results are misinterpreted or not placed in the proper clinical context," they said. "But we believe that this would be a technology which will uniquely improve both sensitivity and specificity of diagnosis."




 Price is 8-20% Lower Than Other
Price is 8-20% Lower Than Other






